Healthcare App Development in India: Cost, Features & Complete Guide
- The Indian Healthcare Digital Landscape
- What Healthcare App Development Actually Means
- Defining the Purpose Before Writing Code
- Core Categories of Healthcare Applications in India
- Step by Step Process for Healthcare App Development in India
- Essential Features for a High Volume and Regulated Industry
- Security for Healthcare Applications
- Technology Stack Considerations
- Healthcare App Development Cost in India
- Compliance as a Competitive Advantage
- Integration Challenges in Indian Healthcare
- Performance and Scalability Planning
- User Experience in Clinical Environments
- Testing and Quality Assurance
- Post Launch Maintenance
- Monetization Models for Healthcare Applications
- Success Stories in Healthcare App Development
- Tips for Founders
- Why Choosing the Right Partner Matters
- Future Trends Shaping Healthcare Technology in India
- Final Thoughts
- About iProgrammer
- FAQs
At 9:40 a.m., the OPD is already full. A patient waits for a lab report that was cleared an hour ago. The lab says it is uploaded. The front desk cannot find it. The doctor refuses to proceed without it. Nobody is wrong. Yet the system stalls. If you have spent time inside a growing hospital or diagnostic chain, you know this scene is not dramatic. It is ordinary. And that is the problem.
India’s healthcare sector is expanding at a pace few other industries can match. According to India Brand Equity Foundation, it is expected to reach over USD 372 billion in 2026. Scale at this level exposes operational gaps fast. What works for one facility breaks across ten locations. Manual coordination fails under volume. Compliance becomes harder. Insurance scrutiny increases.
Healthcare app development in India, therefore, is not a technology trend. It is an operational necessity. The right system aligns doctors, labs, billing, and insurance on a single source of truth.
This guide examines Healthcare app development from a business standpoint. We will look at compliance, security, cost, scalability, and architecture. We will also clarify what separates a capable healthcare app Developer from a vendor who only builds features.
The Indian Healthcare Digital Landscape
India’s healthcare market is complex and uneven. Metro cities operate multi-specialty hospitals with integrated systems. Smaller cities often depend on semi digitized workflows.
Government initiatives like the Ayushman Bharat Digital Mission push standardization. Private health chains push efficiency. Startups experiment with telemedicine, e-pharmacy, and remote monitoring.
However, three structural challenges remain:
- Fragmented patient data
- Limited interoperability
- Strict regulatory expectations
Any serious approach to Healthcare App Development must account for these realities from day one.
What Healthcare App Development Actually Means

Healthcare applications are not generic mobile apps with booking features. They sit inside regulated workflows. They process clinical data. They influence treatment decisions. Healthcare app development includes designing and building applications such as:
- Hospital Management Systems
- Telemedicine platforms
- EHR and EMR systems
- Remote patient monitoring apps
- Diagnostic reporting systems
- Health insurance processing tools
Each type of app has its own set of compliance and integration needs. A reputable healthcare app developer must have a good understanding of clinical workflows before putting a single line of code together.
Medical app development must also involve coordination with doctors, administrators, compliance officers, and IT professionals. Without this coordination, app functionality is reduced to mere decoration.
Many projects fail because founders start with features. Before writing code, leadership must define what operational shift the system should create. Faster billing cycles. Reduced report delays. Lower claim rejections. Better patient retention. The goal must be measurable.
Ask these questions first:
- What operational problem are we solving?
Be specific. Delayed discharge, claim processing backlog, or fragmented patient history are very different problems. - Who uses this product daily?
Doctors, nurses, billing teams, lab technicians, or patients. Each group expects different workflows. - Does it reduce manual dependency?
If staff still relies on spreadsheets or manual reconciliation, the system is incomplete. - Does it integrate with existing systems?
Most hospitals already use some software. Ignoring integration creates duplication and resistance. - Is it compliant with Indian data laws?
Healthcare data carries regulatory responsibility. Compliance cannot be added later.
When objectives are vague, development costs rise and adoption falls. A well structured roadmap reduces rework. It also ensures that the product aligns with hospital realities.
Core Categories of Healthcare Applications in India
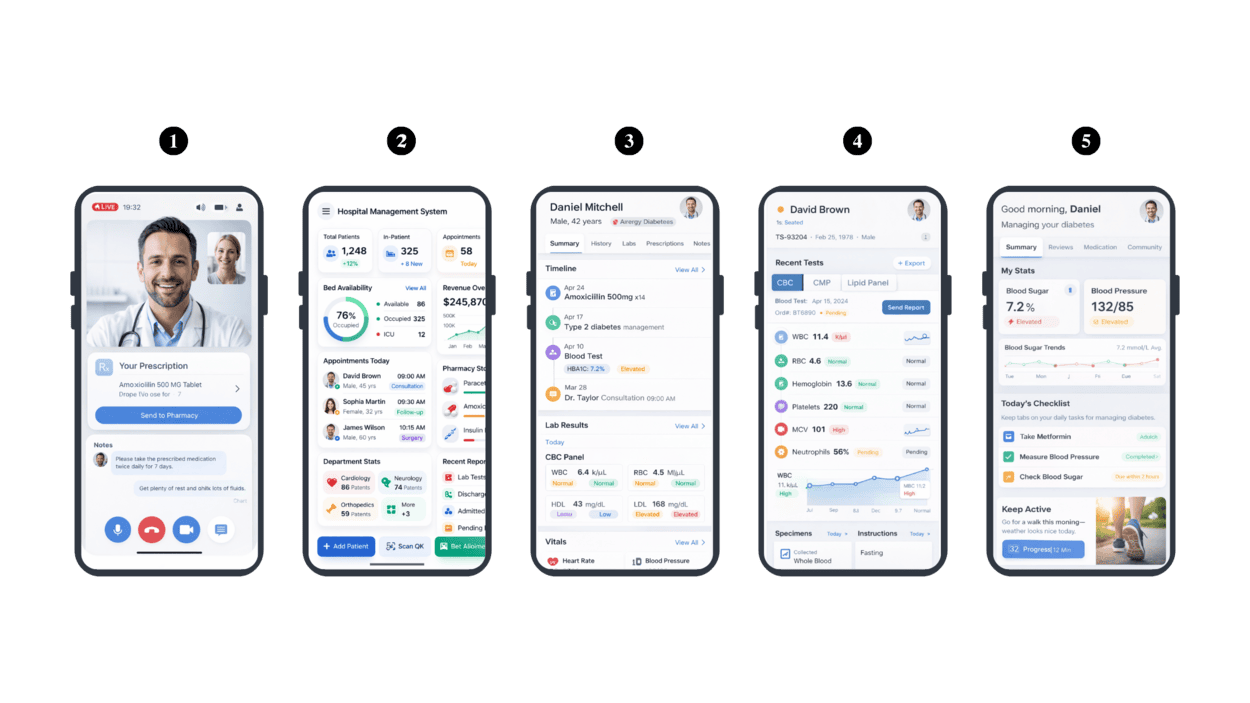
Healthcare is not a single use case. It spans multiple digital needs.
1. Telemedicine Applications
Video consultations, digital prescriptions, follow ups, and remote care tracking. These platforms must ensure secure communication, stable performance, and simple scheduling for both doctors and patients. Examples in India include Practo, Tata 1mg, and Apollo 24|7.
2. Hospital Management Systems
Patient registration, billing, lab integration, discharge summaries, and reporting. These are the operational engines of hospitals and must integrate closely with hospital workflows. Examples include MocDoc and Practo Ray
3. EHR and EMR Platforms
Centralized patient records accessible across departments. These systems improve continuity of care and require structured data management and access control. Examples include Bahmni and global platform eClinicalWorks.
4. Diagnostic and Lab Systems
Test management, automated reporting, doctor dashboards, and patient notifications. Speed, accuracy, and integration with hospital systems are critical here. An example is CrelioHealth.
5. Chronic Care and Monitoring Apps
Diabetes, cardiac, oncology, and mental health management platforms. These are long-term patient engagement, data management, and secure remote access platforms. Examples include BeatO and HealthifyMe
Step by Step Process for Healthcare App Development in India
Healthcare app development should follow a disciplined execution model. Skipping stages creates rework, compliance gaps, and adoption failure. Below is a structured development journey used in serious healthcare implementations.
1. Discovery and Operational Mapping
This stage defines scope with precision. Stakeholder interviews are conducted with doctors, administrators, billing teams, and IT staff.
Existing workflows are documented. Bottlenecks are identified. Integration dependencies are mapped. The outcome of this phase is clarity. Not features. Clarity.
2. Regulatory and Compliance Planning
Before architecture design begins, compliance structures must be defined. Consent mechanisms, data retention policies, audit logging requirements, and access hierarchies are outlined.
Alignment with Indian IT Act provisions and evolving data protection norms is evaluated. This prevents expensive architectural revisions later.
3. Solution Architecture and Tech Stack Finalization
Based on workflow and compliance inputs, system architecture is designed. Mobile, backend, database, and cloud infrastructure decisions are finalized.
Integration layers are defined. Scalability planning is documented. At this stage, performance assumptions are stress tested against projected patient volume.
4. UI and UX Prototyping
Wireframes and clickable prototypes are created. Doctors and staff review the flow before development begins. Feedback is incorporated early.
This reduces resistance during rollout. Clinical environments demand simplicity. Prototypes must reflect that.
5. Development in Structured Phases
Development is executed in modules. Core functionality is built first.
Integrations follow. Security layers are implemented alongside development, not after. Regular sprint reviews ensure business alignment remains intact.
6. Integration and Data Migration
Existing data must be handled carefully. Legacy system data is cleaned, structured, and migrated. APIs are tested under load.
Third party integrations are validated in controlled environments before going live. This stage often determines launch stability.
7. Testing Under Real Conditions
Testing includes performance simulation, security validation, and compliance verification. Load testing reflects real OPD volumes.
Role based access is validated. Vulnerability assessments are conducted. Healthcare testing must mirror real world pressure.
8. Deployment and Controlled Rollout
Instead of a full scale launch, phased deployment is recommended. One department or branch goes live first.
Feedback is gathered. Adjustments are made before scaling. This reduces operational shock.
9. Continuous Monitoring and Optimization
Post launch monitoring tracks uptime, response time, user behavior, and compliance logs. Feedback loops guide feature refinement.
Infrastructure is optimized as usage patterns evolve. Healthcare platforms are not static assets. They are evolving systems.
Essential Features for a High Volume and Regulated Industry
Healthcare products operate in high traffic environments. They also handle sensitive data. Features must support both scale and compliance.
Below is a functional framework that most enterprise healthcare platforms require.
| Layer | Key Capabilities | Why It Matters |
|---|---|---|
| Patient Interface | Registration, booking, reports access | Reduces front desk dependency |
| Doctor Dashboard | Case history, prescriptions, lab view | Improves treatment accuracy |
| Admin Panel | Billing, user roles, audit logs | Ensures operational control |
| Integration Layer | Lab systems, payment gateway, insurance APIs | Enables workflow continuity |
| Compliance Layer | Consent management, encryption, audit tracking | Protects against legal risk |
| Layer | Key Capabilities | Why It Matters |
|---|---|---|
| AI Clinical Support | AI-assisted diagnosis suggestions, drug interaction alerts, predictive risk scoring | Supports faster and more informed clinical decisions |
| Predictive Analytics | Readmission risk prediction, disease progression modeling, population health insights | Enables preventive care and reduces hospitalization costs |
| AI Powered Patient Engagement | Smart chatbots, automated follow-up reminders, symptom triage bots | Improves retention and reduces staff workload |
| Remote Monitoring Integration | IoT device syncing, real-time vitals tracking, anomaly detection | Strengthens chronic care and home-based treatment models |
| Advanced Compliance Intelligence | Automated compliance monitoring, anomaly-based audit alerts | Reduces manual oversight and legal vulnerability |
| Interoperable Health Data Exchange | Standardized health data APIs aligned with national digital health frameworks | Enables cross-hospital data portability and coordinated care |
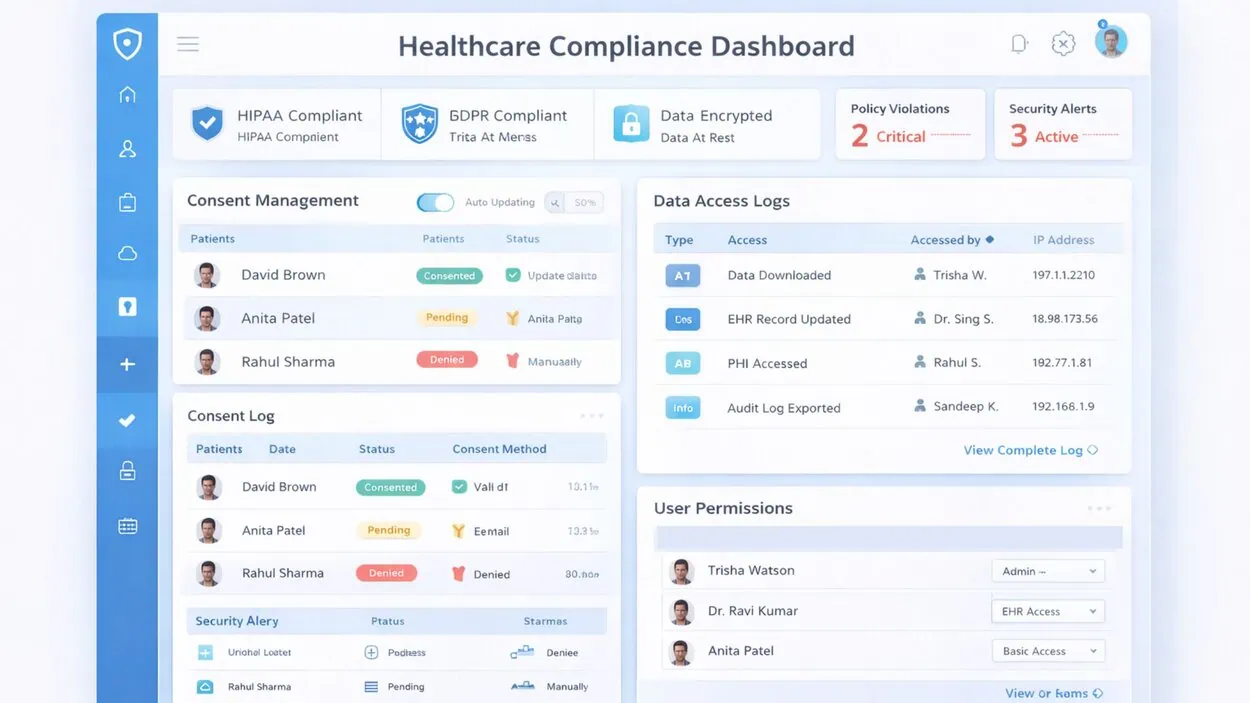
Security cannot be treated as an add on feature. Healthcare data is among the most sensitive categories of information.
| Indian healthcare applications must comply with: | Key security considerations include: |
|---|---|
|
|
Security for healthcare applications must also include periodic vulnerability testing. Static protection is not enough. Threats evolve constantly. A credible healthcare app developer designs security architecture at the database and infrastructure level, not just the UI level.
Technology Stack Considerations
Technology choices directly influence performance and maintenance cost.
1. Mobile Application Layer
This is the interface patients and doctors interact with daily. Performance and stability matter more than visual effects.
- Flutter or React Native for cross platform
These frameworks reduce time to market and development cost. They are suitable for patient apps, telemedicine platforms, and early stage MVPs. However, they require careful performance optimization when traffic scales. - Swift for iOS
Native iOS development offers stronger performance, deeper hardware integration, and better long term maintainability. It is useful when building secure, high reliability clinical applications. - Kotlin for Android
Given Android’s dominance in India, Kotlin ensures better device compatibility and smoother performance. Native Android builds are often preferred for hospital grade applications.
2. Backend Architecture
The backend controls business logic, integrations, authentication, and data processing. This layer must be structured and scalable.
- Node.js
Effective for real time systems such as chat, notifications, and live consultation modules. It handles concurrent requests efficiently when architected properly. - Python
Well suited for healthcare platforms that integrate analytics, automation, or AI driven insights. Frameworks like Django provide structured development and built in security layers. - Java based frameworks
Often chosen for enterprise hospital systems. They offer stability, structured architecture, and long term scalability for complex workflows.
3. Database Layer
Healthcare data is structured, sensitive, and long lived. Database planning must reflect that. Relational databases such as PostgreSQL work well for structured patient records and billing data.
NoSQL databases can support high volume interaction data or flexible schemas. The choice depends on how standardized your clinical data model needs to be.
4. Cloud and Infrastructure
Cloud infrastructure determines scalability and compliance readiness.
Platforms like AWS or Azure provide encryption services, identity management, audit trails, and auto scaling capabilities. However, configuration discipline matters more than provider selection. Many healthcare vulnerabilities arise from misconfigured access controls rather than platform limitations.
Healthcare App Development Cost in India
Cost is one of the first questions founders ask. The honest answer is that pricing varies significantly based on scope. Below is a structured cost estimation view.
| Component | Estimated Share of Budget | Impact on Final Cost |
|---|---|---|
| UI/UX Design | 10 to 15 percent | Influences adoption |
| Backend Development | 25 to 35 percent | Core logic and integrations |
| Mobile App Development | 20 to 30 percent | Patient and doctor interface |
| Security & Compliance | 10 to 15 percent | Regulatory alignment |
| Testing & QA | 10 to 15 percent | Stability and risk control |
| Maintenance | Ongoing | Updates and scaling |
A basic telemedicine MVP may start around INR 15 to 25 lakhs. Enterprise hospital systems may exceed INR 50 lakhs depending on integrations. Cost rises when requirements are unclear or when security is ignored initially.
Compliance as a Competitive Advantage
Many early stage startups see compliance as paperwork. Established healthcare organizations see it as leverage. In a regulated industry, systematic compliance helps to establish credibility with hospitals, payers, and enterprise partners.
- Systematic consent management helps to ensure that patient data use is transparent and auditable. This helps to minimize disputes and maximize patient trust.
- Audit logs create accountability. Each prescription update, report request, and billing modification must be auditable. This helps to minimize liability and maximize internal investigations.
- Systematic and standardized data helps to improve insurance claim processing. Clean data helps to minimize claim rejection rates and maximize approvals.
- Compliance ready systems also move faster in enterprise negotiations. Large hospital chains evaluate risk before features. A system that is compatible with the Indian norms for data protection and healthcare guidelines will often ease the way in overcoming procurement hurdles.
Healthcare systems rarely operate in isolation. You must integrate with:
- Diagnostic lab software:
Automation of reports and tracking of samples are dependent on smooth connectivity. - Pharmacy systems:
Filling of prescriptions and tracking of inventory are dependent on data synchronization. - Insurance claim platforms:
Organized billing and documentation ease approval delays. - Payment gateways:
Secure and organized digital payment transactions are necessary for patient convenience. - Government health registries:
Integration with national or state health registries may be necessary in some cases.
The complexity of integration will often determine the project timeline. An experienced healthcare app developer will be aware of API limitations and legacy system complexities from the outset.
Performance and Scalability Planning
Healthcare traffic spikes are unpredictable. Epidemics, vaccination drives, and insurance campaigns increase load rapidly. Scalable architecture should include:
- Load balancing: Balances server loads to avoid congestion.
- Auto scaling cloud infrastructure: Scales computing resources according to real-time demands.
- Database indexing optimization: Optimizes query performance even as the database grows.
- Caching layers: Prevents repeated database queries for frequently accessed data.
User Experience in Clinical Environments
Doctors do not tolerate friction. Nurses operate under time pressure. Patients vary in digital literacy. Design must be intuitive and minimal.
- Reduce click depth: Critical actions should not require multiple navigation steps.
- Use readable typography: Medical data must be legible across devices and lighting conditions.
- Avoid cluttered dashboards: Highlight essential information. Hide secondary details behind structured navigation.
User experience directly affects adoption rates.
Testing and Quality Assurance
Healthcare testing goes beyond functionality. It includes:
- Data accuracy validation: Ensure reports, billing calculations, and patient records remain consistent.
- Security testing: Identify vulnerabilities in authentication, storage, and API layers.
- Performance testing: Simulate peak loads to evaluate system response.
- Device compatibility testing: Verify stability across varied Android and iOS devices common in India.
- Compliance testing: Confirm alignment with regulatory and audit requirements.
QA cycles must simulate real hospital environments. Skipping this stage increases long term operational risk.
Post Launch Maintenance
Healthcare systems evolve. Regulations change. User feedback emerges. Post launch services must include:
- Security patch updates: Protect against emerging threats.
- Feature upgrades: Adapt to new clinical or administrative needs.
- Cloud optimization: Control infrastructure cost while maintaining performance.
- Compliance audits: Ensure ongoing regulatory alignment.
Monetization Models for Healthcare Applications
Healthcare monetization must balance revenue with trust. Aggressive models damage credibility. Sustainable models align with value delivered.
Below are the most common and practical revenue structures.
1. Subscription Model
Hospitals or clinics pay a monthly or annual fee. This works well for hospital management systems, EHR platforms, and telemedicine software. Revenue becomes predictable. Clients expect continuous upgrades and support.
2. Per User or Per Doctor Licensing
Charges are based on the number of active users or practitioners. Suitable for multi branch hospitals. Costs scale with growth. Smaller clinics can start lean and expand gradually.
3. Transaction Based Model
Revenue is earned per consultation, booking, or processed claim. Common in telemedicine and appointment platforms. Works best when patient volume is high.
4. SaaS with Tiered Plans
Different pricing tiers unlock additional features. Basic plans cover essential tools. Advanced tiers include analytics, AI modules, or integration support. This allows upselling without forcing early complexity.
5. Enterprise Licensing
Large hospital chains prefer fixed enterprise contracts. Includes customization, integrations, SLA guarantees, and dedicated support. Higher revenue per client but longer sales cycles.
6. Commission Model
Platforms earn a percentage from partner labs, pharmacies, or insurance providers. Works when the app acts as a marketplace connector. Transparency is important to avoid trust erosion.
7. Data Insights (Ethically Structured)
Aggregated and anonymized data can support research or operational analytics partnerships. This must strictly follow consent norms and regulatory frameworks. Mishandled data can destroy brand reputation.
8. Remote Monitoring Device Bundling
Revenue comes from pairing software with IoT devices for chronic care tracking. Subscription plus hardware creates recurring value and deeper patient engagement.
INTERVENT International needed a secure platform to drive chronic disease prevention across global medical centers. Manual tracking limited engagement. Telehealth coaching lacked structured integration. Scalability and data security were essential.
We developed a cross platform mobile application with integrated telehealth coaching, personalized health tracking, and structured action plans. Built using Swift UI, Kotlin, .NET, and MySQL, the system supported secure multi region deployment.
- Adopted across 150 plus medical centers
- Improved patient engagement and program adherence
- Secure expansion without performance instability
- If you are planning Healthcare app development, consider these principles:
- Define measurable business outcomes
- Allocate budget for compliance from day one
- Choose scalable infrastructure
- Invest in UX testing with real doctors
- Plan for integration complexity
- Budget for ongoing maintenance
- Technology must serve clinical efficiency. Not the other way around.
Why Choosing the Right Partner Matters

Building healthcare software demands domain understanding. It demands regulatory awareness. It demands architectural foresight. A capable healthcare app developer will:
- Conduct workflow mapping sessions: They spend time understanding admission flows, discharge cycles, lab coordination, and billing approvals before defining architecture. This prevents costly rework later.
- Recommend compliance structures: They embed consent management, audit logging, and role based access at the system level rather than adding them as afterthoughts.
- Design scalable architecture: They plan for multi location expansion, higher patient volume, and integration growth from the start.
- Provide documentation for audits: Clear technical and process documentation simplifies regulatory reviews and enterprise procurement evaluations.
- Offer long term support: Healthcare systems require continuous updates, monitoring, and optimization. A partner must commit beyond launch.
Future Trends Shaping Healthcare Technology in India
India’s healthcare sector is moving from basic digitization to structured digital ecosystems. The shift is practical and policy driven.
1. Standardized Digital Health Records
Unified and interoperable electronic records are becoming the norm. Structured patient data will soon be expected across hospitals and networks, not treated as an upgrade.
2. AI Assisted Diagnostics
AI is supporting imaging, pathology screening, and early risk detection. Adoption is rising in high volume specialties where speed and precision matter.
3. Remote Monitoring as Routine Care
Chronic disease management is extending beyond hospital visits. Remote tracking tools are improving follow ups and reducing inpatient load.
4. Predictive and Preventive Intelligence
Medical app development will increasingly embed predictive analytics for risk scoring and proactive care. However, these capabilities depend on stable, secure, and well structured core systems.
Healthcare technology should reduce friction, not add complexity. It should support doctors, empower patients, and protect data.
Healthcare app development in India demands clarity, discipline, and regulatory awareness. It demands structured planning before coding begins.
When executed properly, healthcare applications improve operational speed, transparency, and patient satisfaction. They also create measurable business value.
At iProgrammer, we approach healthcare technology with operational seriousness.
- Workflow Before Features
We map admission cycles, lab coordination, billing flows, and discharge processes. Architecture follows real hospital movement. - Compliance From the Start
Consent tracking, audit logs, and role based access are structured into the core system. Security is foundational, not optional. - Built to Scale With Growth
Infrastructure is planned for rising patient volumes and multi location expansion. Systems should grow without structural redesign. - Long Term Stability Focus
Clean architecture, structured documentation, and disciplined testing reduce technical debt and future risk.
We design and build both layers as one connected ecosystem. Our web application development capabilities support complex dashboards, integrations, and administrative controls. Our mobile app development expertise ensures secure, high performance patient and doctor applications.
When both layers are architected together, data flows cleanly, performance remains stable, and compliance stays consistent. That alignment determines whether a healthcare system simply launches or continues to perform under real world pressure.
What are the benefits of Healthcare Applications?
How long does it take to develop a Healthcare App?
How can people with disabilities use my Healthcare App?
What are the key considerations while making a Healthcare App?









